Uses of antibiotics in livestock production: Pros and cons

The following provides an overview of the uses of antibiotics in livestock farming, with a particular focus on the advantages of these products in terms of animal health and production.
Uses and mode of action
Antibiotics are used in veterinary medicine for therapeutic purposes by administering them in water or by injection to overcome certain infections, such as mastitis in dairy cattle, septicemia following badly infected wounds, peritonitis, etc. Abdominal and other surgery have also been rendered safer through the use of antibiotics.
In these cases, antibiotics inhibit or kill susceptible bacteria in 3 ways broadly:
Disruption of microbial cell wall synthesis (e.g. penicillin and bacitracin);
Affecting the cell membrane, in the way of detergents (e.g. polymixin, novobiocin and nystatin); and
Interfering with protein synthesis in bacteria (e.g. tetracycline, chloramphenicol, neomycin, streptomycin and erythromycin).
Antibiotics are also used at a sub-therapeutic level to promote growth and improve the feed efficiency of animals. Here they may be used either as feed additives or through implants, but at a lower dosage than for therapeutic purposes.
Efficacy criteria
To be useful in veterinary medicine an antibiotic must have the following properties:
powerful action in the body against one or more strains of bacteria;
specific action;
low toxicity for tissues;
be active in the presence of body fluids;
not be destroyed by tissue enzymes, such as trypsin;
be stable;
not be too rapidly excreted; and
ideally, not give rise to resistant strains of organisms.
Antibiotics and nutrient requirements
Antibiotics have been shown to enhance the utilisation of certain nutrients, such as protein, vitamins and minerals. This effect may be indicative of the nutrient-sparing effects of antibiotics and improvement of the uptake of nutrients from the intestinal tract which, in turn, leads to reduced nutrient requirements, depending on how the post-absorptive utilisation of the nutrients takes place.
Effects on animal performance
Dairy cows
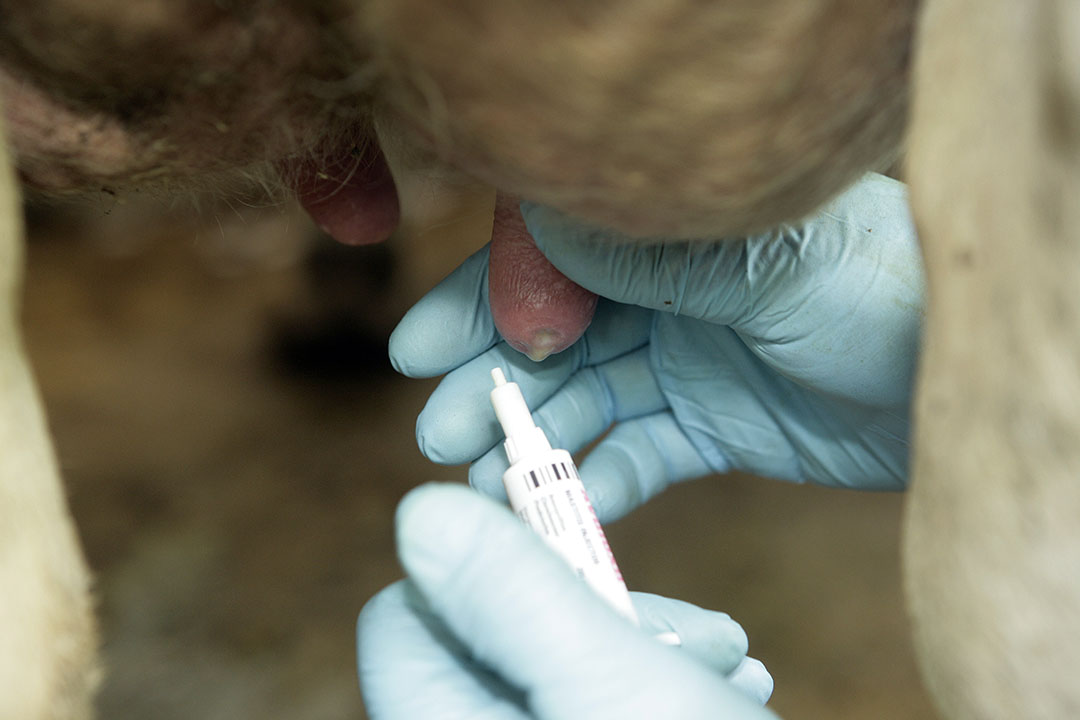
It is a sound decision to have all cows routinely treated at the time of drying off with an antibiotic that has been specifically formulated for this purpose. This simple routine measure does not contaminate saleable milk with antibiotics and it will remove 60-70% of existing infections, as well as prevent most new infections that are common in the early part of the dry period. In addition, cows with clinical mastitis at any stage of lactation should be treated with an antibiotic. The specific antibiotic for use during lactation and dry cow therapy should be discussed with a veterinarian who is familiar with the herd.
Calves
The inclusion of antibiotics (e.g. chlortetracycline, aureomycin or spiramycin) in starters for early weaned calves at 20-40 mg or per kg of starter has generally increased feed intake, feed efficiency and growth. The enhancements in growth rate during the first 16 weeks of age have ranged from 10% to 30%, although in a few studies no growth promotion occurred. It was suggested that antibiotics in the starter have a protein-sparing effect since a growth response was obtained only when protein intake was limited. A greater growth response was noted when adding antibiotics to the starter compared with adding it to the milk replaces for early weaned calves. In addition, antibiotics have a scours-preventing effect and improve calves’ well-being.
Beef cattle
Studies on the use of chlortetracycline or oxytetracycline for beef steers showed that at 75-150 mg per head per day there was a substantial increase in growth rates without adverse side effects. The increased growth in this case was probably due to the effects of these antibiotics on rumen fermentation and increasing the molar ratio of propionate-to-acetate which helps enhance the growth of animals because of the greater energy value of propionate compared to that of the acetate (the energy value of propionate is 2.4 times higher than that of acetate). Studies show that the use of such antibiotics increases the dressing percent and other carcass traits, but as yet no elucidation is available of the mechanisms by which antibiotics affect carcass quality.
Problems associated with the use of antibiotics
Using antibiotics too often or for the wrong reasons can change bacteria so much that they no longer work in combating certain infections, even the most powerful antibiotics available. This is called bacterial resistance or antibiotic resistance and in these cases infections are harder to treat than those caused by non-resistant bacteria. Resistant pathogens in animals may transmit to humans through antibiotic residues present in products from treated animals and cause symptoms, such as vomiting, nausea, bloating, indigestion and abdominal pain, with higher treatment costs, prolonged hospital stays and increased mortality.
Antibiotics may also affect soil function and plant composition. In soils exposed to the manure of antibiotic-treated animals negative effects on the micro-organisms involved in normal soil processes are seen, such as nitrification and organic matter decomposition. When corn, potatoes, lettuce and other crops used for human consumption are planted, there is an uptake of antibiotics by the plant tissues, reaching a concentration of about 0.1 to 1.2 ppm on a dry weight basis. Although such concentrations are not toxic, over time this may increase the development of antibiotic resistance in humans consuming these crops.
Alternatives to antibiotics
A reduction in antibiotic usage in farm animals can be achieved through a careful combination of antimicrobial peptides, pre and probiotics, in-feed enzymes, plant extract (oregano, cinnamon, Mexican pepper, thyme, oregano and garlic extract), phytochemicals (essential oils or tannins) and organic acids (citric or acetic acids). These agents have been successfully applied to disease models of cattle and mono-gastric animals at comparable costs but with better herd surveillance and fewer risks to animals, humans and the environment. A suitable level of veterinary control and economic analysis, however, is recommended before selecting any of these agents, along with proper animal management, nutritional measures and biosecurity programmes.
References available from the author on request.











